
The temporal resolution of 8-frame ECG SPECT as the authors point out is 5.6°. This is a small study of predominantly non-ischemic patients in which outcomes were not assessed. The manuscript is a step in right direction but there are several shortcomings in both the technique and the study, which should be kept in mind for any future work. Third and most interesting finding is the recommendation of the anterior lead placement in close to 55% of the patients, which would be a major departure from the current practice in which the posterolateral segment is usually targeted for LV lead placement. (2) More than one segment was recommended in close to 45% of the patients as segments whose phase angles were within 10° of the latest phase angle were considered optimal for lead placement. However, inter-operator reproducibility of the segment of choice by automatic method was less than 70%. There are three noteworthy findings in this manuscript: (1) There was an excellent agreement between the automatic method by the first operator and the visual integration method by experts. Automatic assessment was then compared with the visual integration method by experts. The latest contracting, which did not have scarring, was recommended for LV lead placement. Data from perfusion assessment were used to identify scarred segments. Phase analysis as described above was then used for dyssynchrony assessment. In their study, the authors acquired images using 8-frame ECG-gated SPECT in 36 patients predominantly with non-ischemic cardiomyopathy and QRS duration >120 ms. The current study 10 by Zhou et al helps in taking personalized CRT one step closer by trying to automate dyssynchrony assessment. This can then be combined with viability assessment and potentially fused with coronary sinus venograms, 9 thereby providing a road map for precise and individualized LV lead placement. Phase standard deviation and phase histogram bandwidth can then be used to quantify dyssynchrony and also to identify the latest contracting segments. This information of phase of onset of contraction is displayed on a polar map. 8 It uses Fourier harmonic function to approximate change in thickness of myocardium during a cardiac cycle to onset of contraction. Phase analysis from gated SPECT imaging has been proposed as a relatively straightforward way of assessing dyssynchrony. The largest trial using echocardiographic dyssynchrony assessment-guided CRT placement was negative 6 although the inclusion criteria included only narrow QRS patients. There is disagreement on which echocardiographic parameter to use for dyssynchrony assessment and reproducibility has been poor. Single-Photon Emission Computed Tomography (SPECT), Echocardiography, and Cardiac Magnetic Resonance Imaging (CMR) all have been evaluated for this purpose and each has its own limitation. 5, 6, 7 Ideal imaging modality will have high spatial and temporal resolution to accurately identify the latest contracting segment, will give the implanting physician information about myocardial viability, coronary venous anatomy, and will have high degree of automation and reproducibility. 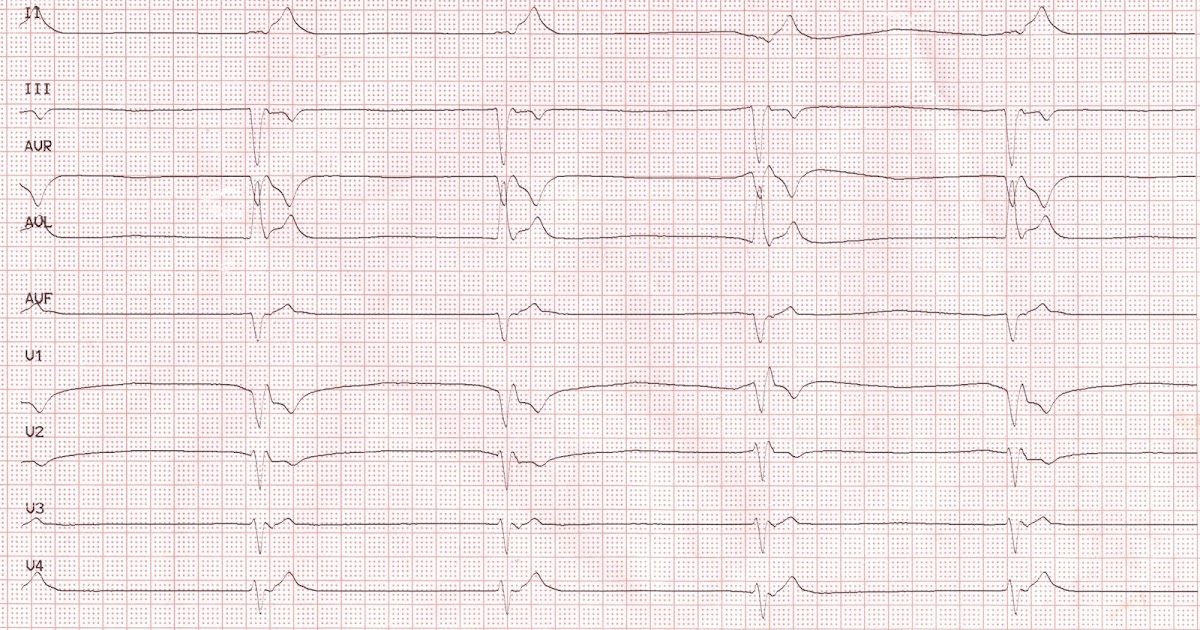
Several studies have tried to address one or more of these questions using different imaging modalities. In the presence of typical LBBB, latest activating segment is posterolateral basal left ventricle (LV) and there is usually significant dyssynchrony. To overcome these challenges and improve patient response, implanting physician will benefit from the following information: (1) Is there the presence of significant dyssynchrony? (2) Which is the most dyssynchronous segment of the left ventricle? (3) Can that segment be accessed and used for pacing? This information will be most useful in patients with intraventricular conduction delay (IVCD) and atypical LBBB like QRS pattern rather than typical LBBB. 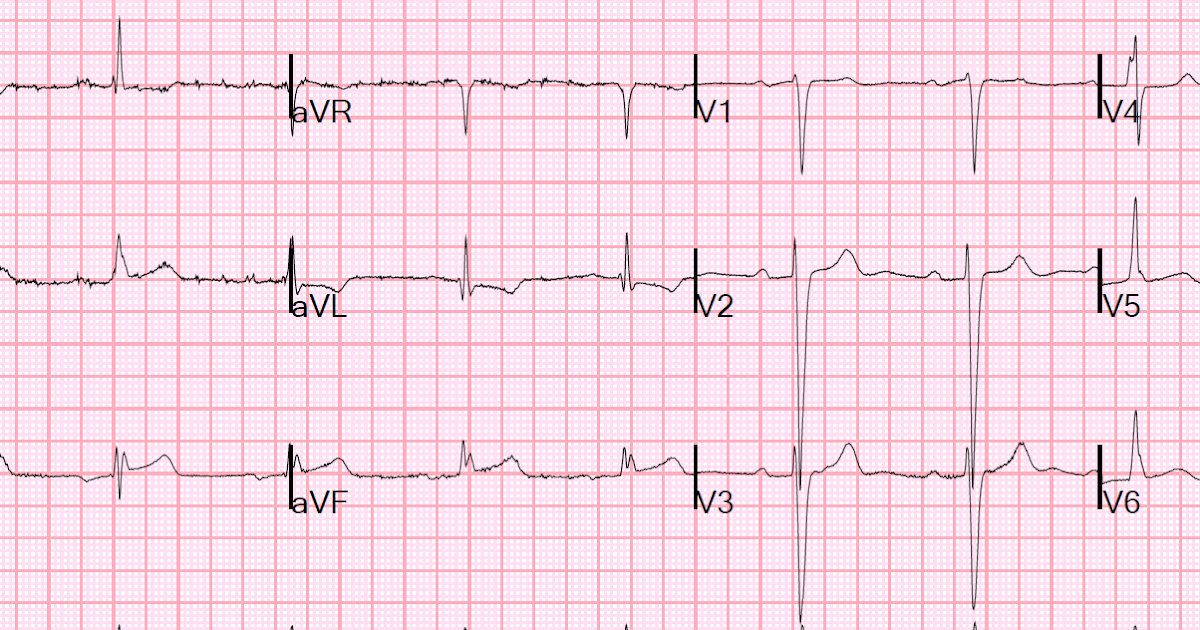
The reason for this poor response rate is multifold including lack of dyssynchrony, presence of scar at the site of lead implantation, and inappropriate LV lead position. In those who lack these criteria response rate to CRT has been poor. Response rate is much higher in individuals with typical left bundle branch block (LBBB) QRS morphology, with QRS duration >150 msec and non-ischemic cardiomyopathy. Using these guidelines, 60-70% of the CRT recipients respond with improvement in symptoms and/or ejection fraction. 1, 2, 3 CRT trials’ inclusion criteria have been based solely on QRS duration with left ventricular (LV) lead implantation in the posterolateral branch of the coronary sinus as the preferred location. Cardiac resynchronization therapy (CRT) in appropriately selected patients can significantly improve left ventricular function and New York Heart Association (NYHA) class.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
